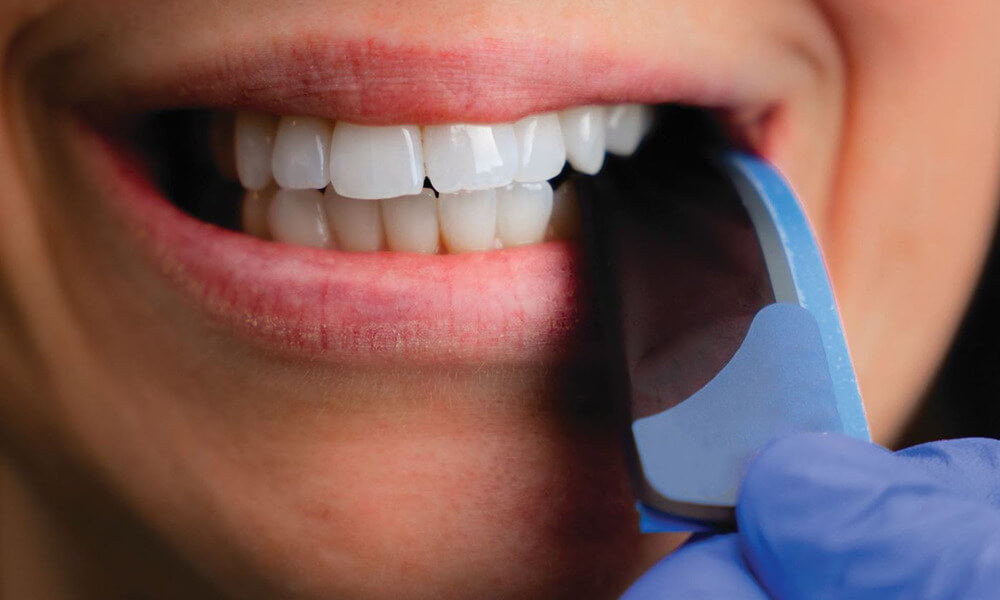
Changing VDO and Correcting Resultant Lisps
Many times, we need to increase the vertical dimension of occlusion (VDO) to put teeth where they should be esthetically and restore teeth that are severely worn from attrition or erosion. If you are concerned that changing VDO will cause joint or muscle pain, put your mind at rest. My experience is that it won’t. If you are concerned it will cause pain, put that thought aside too. My experience is that it won’t.
We want to change the vertical dimension only as much as we needed to accomplish the esthetic and functional goals of the case. That will minimize the effect changing VDO may have phonetics.
Phonetics May Be a Challenge
Vertical dimension has impact on two phonetic sounds in particular—F, S and V. F and V are similar. When we say them, we touch the edge of our upper central incisors just on wet-dry line on the inside of our lower lip. Saying F and V has to do with mandibular lip position, and the patient learns to adjust that position when VDO is changed. In my experience, they adjust to this in two to four weeks. They learn to accommodate a new mandibular position that touches the lower lip more gently.
S is a totally different sound. People say S in one of three different ways.
- Some people make the sound S by making a small air space that’s between their upper and lower incisors edge to edge.
- Some people make the sound S by making that same small air space but with their lower incisal edges just lingual to their upper incisal edges.
- Some people make the sound S by making that same small air space but with their lower incisal edges just labial to their upper incisal edges. And those are our Class 3 occlusion patients.
The air space needs to be a precise amount of distance. If you have too little space, the patient lisps. If you have too much space, the patient spits or sprays saliva. Neither of which the patient is happy about. If the patient is totally edentulous, the patient may adapt to the new VDO of their prostheses, but patients rarely adapt to correct their pronunciation of S if they have a new VDO on natural teeth. This means we need to be careful about altering VDO.
The only way to test if a patient will have a lisp or other phonetic challenge is to test the VDO with provisionals, not with a removable bite splint.
Correcting Lisps Created by Anterior Restoration
How much air space do patients need to pronounce S without a challenge? They need about 100 microns to not lisp or spray saliva. To correct for too large or too small a space, I learned the following trick I hope you find helpful.
Madam Butterfly Silk is about 94 microns thick. I have the patient sit up and hold the silk between their upper and lower incisors with a Miller forceps. While the articulator silk is between the teeth, I have the patient count from 60 to 70. As they count the entire series of numbers, they relax into the process and red ink is transferred to their incisal edges if the space is smaller than 94 microns. If we see red marks, including on the canines, we need to increase the air space. My experience is that it takes four to six passes with the articulator silk and patient counting from 60 to 70 to adjust the airspace sufficiently. As you are doing this, the patient experiences the positive benefit of the lisp going away. I then tell the patient to go home and “observe how you sound. Ask others how you sound. We may need to do a little more refinement.”
If the patient lisps edge to edge, I shorten the lower incisal edges because upper incisors are esthetic. If the patient says S with the lower incisors lingual and they have red marks on their lower lingual and on their upper labial, I pick the upper or lower incisors and make adjustments where they are structurally and esthetically least impactful. If they are Class 3 and say S with their lower incisors, labial to their upper incisors, I always adjust the lingual marks on the lower incisors.
Related Course
Direct Composite: Predictable, Easy and Beautiful
DATE: October 25 2024 @ 8:00 am - October 26 2024 @ 4:00 pmLocation: The Pankey Institute
CE HOURS: 14
Regular Tuition: $ 2195
Single Occupancy with Ensuite Private Bath (per night): $ 290
Achieving Predictable and Stunning Anterior Results Direct composite is something we do every day in our practices. Yet, they can sometimes be frustrating when we don’t get a tight contact…
Learn More>







That was very useful.